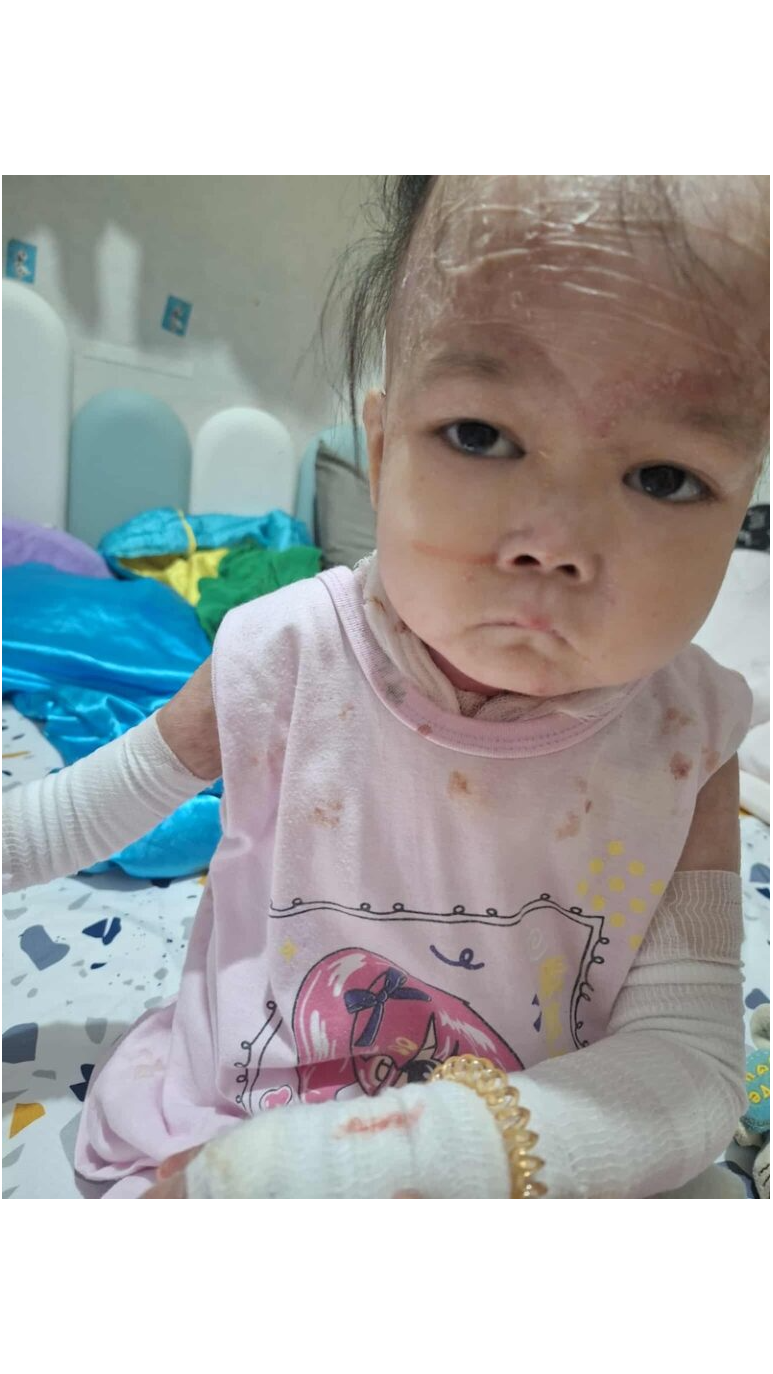
Key Takeaways
- Fragility of “Butterfly Skin”: Epidermolysis Bullosa (EB) causes skin to be so delicate that minor friction or gentle touches can create life-threatening blisters and wounds.
- High Mortality Rates: Infants with severe forms of EB may not survive their first birthday, and the general life expectancy for those with chronic forms is often under 30 years.
- Intensive Daily Care: Management involves grueling, hours-long bandage changes that cause severe pain and additional trauma to the skin.
- Direct Medical Support: Children require specialized bandages, severe pain medication, and nutritional support to survive the daily complications of the disease.
- Direct Impact: Specialized relief programs currently provide life-saving care to over 5,100 children worldwide who are otherwise medically neglected.
The experience of a newborn baby in agony from a simple diaper change, or a parent unable to hold a child’s hand because the contact causes skin to peel, is the daily reality for families affected by Epidermolysis Bullosa. This genetic condition transforms basic physical affection into a source of physical trauma.
When a Gentle Touch Becomes Dangerous
Epidermolysis Bullosa turns everyday interactions into hazardous encounters. A caress, an embrace, or even the friction from soft clothing can tear away layers of skin, creating wounds that may take weeks or months to heal. This genetic defect prevents essential skin proteins from forming proper bonds between the epidermis and dermis, leaving children with skin often compared to the wings of a butterfly.
Caregivers quickly learn that showing affection requires extreme caution. Acts such as picking up a child or changing their clothes are treated as meticulous medical procedures. Any slight miscalculation in handling can result in new blisters, increased pain, and the risk of life-threatening infections.
The Butterfly Children: Why Skin Fails
Genetic Defects and Fragile Bonds
The root cause of this condition lies in mutated genes that fail to produce essential skin proteins. These proteins are responsible for creating the structural anchors that connect the two main layers of the skin. Without these molecular bonds, even minimal pressure causes the layers to separate, resulting in painful blisters filled with fluid or blood.
Medical experts have identified more than 30 subtypes of the disease. Some mutations impact the basement membrane zone, while others affect the proteins that hold individual skin cells together. This genetic diversity explains why symptoms range from localized blistering to complete skin loss across 80 percent of the body.
From Birth to Life-Threatening Wounds
The moment infants with this condition are born, medical teams must exercise extraordinary care. Standard delivery and cleaning procedures can strip away large patches of a newborn’s skin. Hospital staff often identify the condition when routine handling causes unexpected blistering, leading to immediate genetic testing and specialized wound care protocols.
What appears as an external skin issue is often a systemic challenge. Internal organs are also affected, with blisters forming in the mouth, throat, and digestive system, making eating and swallowing extremely difficult for the child.
Daily Reality for Affected Families
1. Grueling Bandage Changes
Families face a constant paradox: the treatments necessary for healing cause additional trauma. Daily bandage changes can take three to four hours and require severe pain medications. The specialized dressings required for these wounds are designed to be non-adherent, yet the removal process remains a significant source of physical and emotional distress.
Parents must become specialists in wound care, learning to apply specialized dressings, manage infections, and administer therapeutic nutrition. Many describe the psychological toll of performing procedures that their children perceive as painful, even though they are necessary for survival.
2. The Impact of Minimal Contact
The “no touch” reality is often the most emotionally devastating aspect for families. Medical guidelines emphasize minimal contact to prevent further skin loss. Children learn early that physical touch is associated with pain, which can create barriers to social development and traditional emotional bonding.
Siblings may struggle to understand why they cannot play normally with an affected brother or sister. Family dynamics frequently shift toward the protection of the child’s skin, leading to isolation. Standard childhood activities like visiting a playground or participating in sports are generally impossible for these children.
3. Internal Blistering and Nutritional Needs
The condition extends beyond visible skin wounds. Blisters inside the mouth make eating painful, and the esophagus can develop strictures from repeated scarring. Many children require feeding tubes and highly specialized nutrition to prevent malnutrition and dehydration.
Chronic blood loss from open wounds frequently leads to severe anemia, which may necessitate blood transfusions or intravenous treatments. This combination of poor nutrition, chronic pain, and repeated medical interventions creates a cycle of health challenges that requires constant, high-level medical support.
Severe Forms: The Fight for Survival
Infant Mortality
Severe variants of the condition can be devastating. Infants may be born with widespread skin loss, creating massive wounds that cover a significant portion of their bodies. The extensive damage leads to fluid loss, electrolyte imbalances, and high risks of overwhelming infection that can prove fatal within the first year of life.
While medical teams provide supportive care, underlying genetic defects make natural healing difficult. These cases underscore the urgent need for funding research into systemic cures and providing immediate medical supplies to manage symptoms.
Reduced Life Expectancy
Those who survive infancy still face significantly shortened lifespans. The constant cycle of blistering and infection takes a cumulative toll on the body. Many patients develop aggressive skin cancers or secondary health conditions, such as tumors or heart complications, by their teens or twenties.
The Challenges of Funding and Research
Orphan Disease Status
Because this is a rare genetic condition, it has historically faced challenges in securing research funding and public awareness. Major pharmaceutical investments are often directed toward conditions affecting larger populations, leaving those with rare diseases with limited treatment options.
As a result, many families, particularly in underserved regions, lack access to the most basic life-saving care. This has created a global crisis where children suffer from medical neglect because their condition is not covered by major international charities.
A Specialized Path to Relief
According to specialists, addressing this crisis requires a dual approach. While funding research for a cure is vital, there is an immediate need to provide medical supplies to children suffering today. By prioritizing immediate intervention, children in poverty-stricken countries receive the bandages and medication they need to survive.
Advancements in Research Funding
Ongoing research is investigating systemic treatments that address the root genetic causes of the disease. These include studies into gene therapy and molecular research aimed at reducing inflammation and promoting skin stability.
Recent initiatives have focused on making these potential treatments affordable and accessible to a global population. The goal is to develop solutions that can be delivered to children in developing countries, ensuring that a future cure is not limited by a family’s financial status.
Real EB Cases Show Ongoing Struggles
Baby John’s Story: Survival Against the Odds
Baby John’s case illustrates the extreme fragility of life for newborns with EB. He was born with life-threatening wounds that left him with no skin from his ribs to his toes. His survival underscores the critical importance of immediate medical intervention and the delivery of specialized wound care supplies during the first days of life.
Lily’s Journey: The Challenge of Internal Blistering
For children like Lily, the condition extends far beyond external skin wounds. Lily suffers from painful blisters inside her mouth and throughout her digestive tract. This makes the simple act of swallowing food an excruciating process, requiring specialized therapeutic nutrition and constant medical monitoring to prevent malnutrition and secondary infections.
Measurable impact is demonstrated through monthly fund delivery and video updates from children like Baby Joyce, who rely on donors for their daily supply of specialized bandages and medication. Specialists in the field emphasize that while a future cure is the long-term goal, the children suffering now cannot wait. Providing “butterfly children” with the medical supplies necessary to stop excruciating pain is the most immediate way to save lives.
The Role of Direct Support
For children living with Epidermolysis Bullosa, direct support can mean the difference between constant suffering and a chance to survive. Specialized bandages, pain medication, nutritional care, and infection treatment are not optional comforts but daily necessities for managing this devastating condition. When families in underserved regions receive these life-saving supplies, children are given immediate relief from extreme pain and a better chance to endure the ongoing complications of EB.
No Baby Blisters
731 Chapel Hills Drive
Colorado Springs
Colorado
80920
United States


